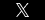Your daughter accompanies you to a doctor’s appointment for moral support, and the doctor addresses all his questions to her instead of to you.
Your daughter accompanies you to a doctor’s appointment for moral support, and the doctor addresses all his questions to her instead of to you.
Nothing like feeling invisible!
The nurse talks to you the way Kindergarten teachers speak to their students, sometimes using the “royal we” and often using inappropriate terms of endearment like “young lady” or “young man.”
How insulting!
You go to a healthcare professional for a specific issue and are either made to feel like you’re making a big deal out of nothing or are sent for a battery of unnecessary tests.
Each of these scenarios is an example of how ageism manifests in our healthcare system. It’s a ubiquitous and often insidious issue that demeans seniors, creates very real health risks, and—according to a 2018 study by Yale University Professor Becca R. Levy—costs the U.S. $63 billion annually.
What is ageism?
Ageism is a systemic form of oppression and discrimination based on a person’s age. Ageism can affect people of all ages, but tends to be especially prevalent against older people. In some cases, ageism is a subconscious bias; but in other cases it is explicit and even hostile.
A study published in The Gerontologist found that ageism is a problem in healthcare settings around the world, and it affects every element of the healthcare experience from diagnosis to treatment and from institution-level healthcare policies to organizational workplace culture.
As the examples above demonstrate, ageism can take many forms. Patronizing baby talk—sometimes referred to as “elderspeak”—may seem like a minor annoyance, but can have very real effects on a patient’s ability to speak up or be heard. At the other end of the spectrum, a nurse or other caregiver might ignore an older patient almost entirely, treating them as almost a non-human entity. Other ageism-related issues, such as undertreating or overtreating, can have very real health and financial implications. In extreme cases, ageism can lead to neglect and abuse.
Where does ageism come from?
People, including healthcare professionals, who behave in an ageist way usually do so because they make incorrect assumptions about aging and carry certain biases or prejudices toward older people. They simply do not have a deep enough expertise about aging to know how to handle patients more appropriately. They may assess a situation or make treatment recommendations based on their own assumptions about what’s to be expected as we age, and those assumptions can be inaccurate.
Ageism can also be the result of frustration. It can take extra patience to help an older person understand the complexities of a medical concern. Instead of taking the time to walk elderly patients through all the details, healthcare professionals can rush through a consultation, providing only cursory information.
How to address ageism
There are a number of ways to address ageism when you encounter it in a healthcare setting. Which option you choose depends on the situation and the overall stakes.
If, for instance, a healthcare provider engages in elderspeak during an appointment, you can choose to ignore it, confront it directly, or try to diffuse the situation with humor while still making your point.
- Confronting it might sound something like, “I am not comfortable with you calling me ‘dear,’ and would prefer that you call me Mrs. Owens.”
- Diffusing the situation might sound something like, “I appreciate you calling me a ‘young lady,’ but I haven’t been young for many years now. You can just call me Janice.”
- If you choose to address ageism in any way, it’s best to use “I statements” that describe how you feel rather than “you statements” that point the finger at the other party.
A firmer approach may be required if the ageism you’re dealing with is affecting your treatment and health outcomes. One of the things that makes ageism so hard to deal with is that many older people have internalized ageist beliefs. They end up assuming that whatever is wrong is their fault.
It’s important to trust your instincts and remember that you have a right to the healthcare provider’s time and to ask whatever questions you have. If it helps, bring along someone who can offer moral support. Or you can practice what you want to say with a friend before you go to your appointment.
Ageism is a big problem, but there are small steps we can take every day.
Ultimately, ageism is a huge, systemic issue that affects elderly people all over the world. It will take a great deal of education and even legal and policy changes to bring about widespread change.
In the meantime, individuals can make a difference. Whether a person is a senior seeking medical services or a healthcare provider serving seniors, everyone has the ability to learn more about ageism and be more mindful about how their interactions affect others.
It’s not always easy to speak up, but using your voice to combat ageism in healthcare can help not only you, but also others who experience similar discrimination and might not be ready to speak up for themselves.
Related Posts:
Positive Aging: Why it Matters and Where to Start
Being a Healthcare Advocate: How to Best Engage with Healthcare Professionals
How to Close the Communication Gap with Older Adults
When the Child Becomes the Parent: 5 Tips to Ease the Transition
 Connecticut Estate Planning Attorneys Blog
Connecticut Estate Planning Attorneys Blog